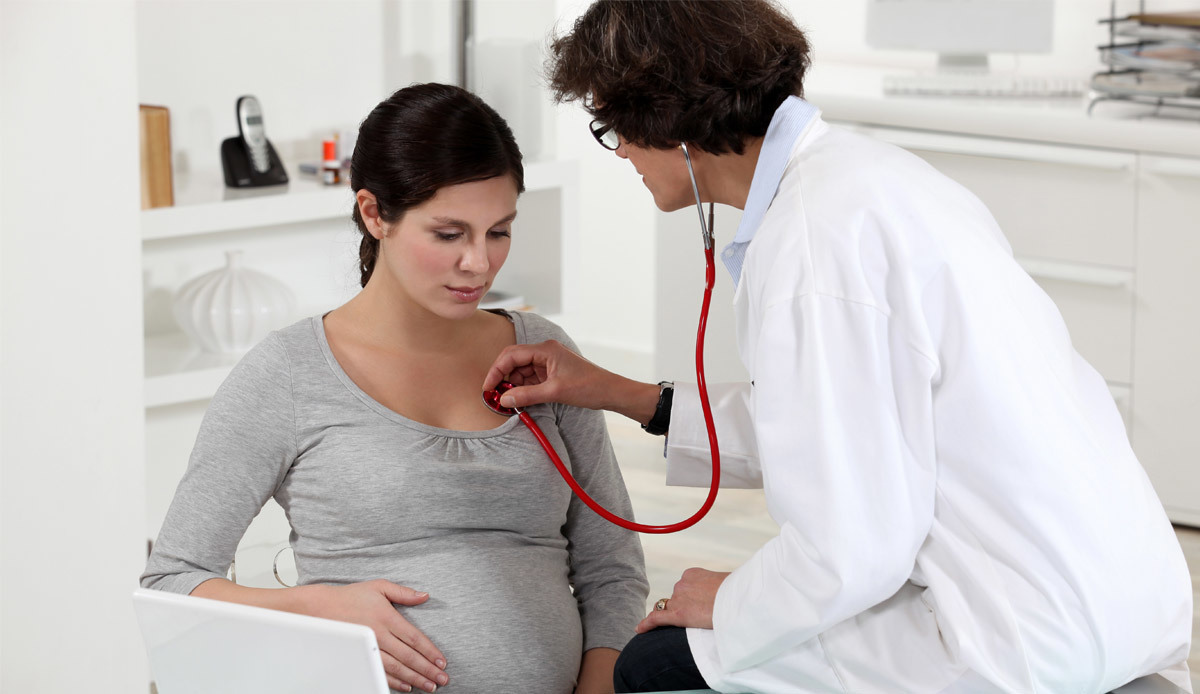
 Using IVF, artificial insemination and other forms of assisted reproductive technology to conceive can be very expensive. Artificial insemination (ICI or IUI) with the use of donor sperm can cost anywhere from $500 – $1500/cyle or more. The average cost in the United States for IVF appears to be $13,000 – $15,000 per cycle, or more, depending on the type of treatment, testing, and medications needed. As such, it is important to become familiar with the costs of infertility treatment up front and determine whether these costs are covered by insurance or must be paid out of pocket.
Using IVF, artificial insemination and other forms of assisted reproductive technology to conceive can be very expensive. Artificial insemination (ICI or IUI) with the use of donor sperm can cost anywhere from $500 – $1500/cyle or more. The average cost in the United States for IVF appears to be $13,000 – $15,000 per cycle, or more, depending on the type of treatment, testing, and medications needed. As such, it is important to become familiar with the costs of infertility treatment up front and determine whether these costs are covered by insurance or must be paid out of pocket.
Insurance policies dictate whether there is coverage related to infertility. Individuals attempting to get pregnant via artificial means are well advised to review their policy language closely to determine the scope of coverage, if any. To determine whether infertility care is covered and the scope of coverage, it is best to obtain a full copy of the insurance policy, rather than just a summary document that may be provided by the employer.
Fifteen states have adopted laws mandating some form of insurance coverage for infertility: Arkansas, California, Connecticut, Hawaii, Illinois, Louisiana, Maryland, Massachusetts, Montana, New Jersey, New York, Ohio, Rhode Island, Texas, and West Virginia. While some of these laws provide significant detail on the type of procedures covered and the scope of coverage, other are much more vague. At one end of the spectrum are states like Connecticut and Illinois which require certain individual and group plans to provide coverage for a relatively broad range of infertility treatments, including artificial insemination, IVF, GIFT, ZIFT and low tubal ovum transfer. At the other end of the spectrum are states like Montana and West Virginia, which require HMOs to cover infertility services but do not define “infertility.”
A more detailed state-by-state summary of laws relating to coverage for infertility treatment can be found at www.resolve.org.